Dr. Phil Zeltzman’s Blog
Puppy Magic, my biggest ethical dilemma of 2020
Puppy Magic, a now 13 year old Labrador, never knew that he was my biggest ethical dilemma last year. He has a very interesting story and a long journey…

In June of 2019, Puppy Magic had a TPLO to treat a tear of his left ACL. This is my most common surgery by far, so it was supposed to be straightforward. But when a nurse placed a tube in Puppy’s windpipe at the beginning of anesthesia, a mass was noticed in the very back of his mouth. A biopsy of the mass was sent to the lab. The TPLO surgery went well and Puppy went home smoothly.
A week later, the biopsy returned as a malignant melanoma, an aggressive type of cancer.
You could say that it was an accident that the nurse noticed the mass. I firmly believe that it was not. It was found because of the attention to detail and experience of the anesthesia nurse. Not only did she notice the mass, but she alerted her vet who acted on it.
Puppy’s very dedicated owner, thankful that the cancer was caught so early, went to consult with a cancer specialist (oncologist). Incredibly, melanoma can be treated with a vaccine in dogs. Puppy responded well to the treatment and went into remission.
Over a year later, Puppy Magic was taken to the ER because of a limp in the right back leg. A torn ACL was diagnosed – again. In addition, Puppy Magic showed signs of laryngeal paralysis, i.e. difficulty breathing. The ER doctor told the owner that he didn’t recommend addressing the ACL tear or the breathing difficulty in a dog with oral cancer.
When I heard about it, that put me in a very delicate situation.

What was I supposed to do?
Say nothing, and allow my patient to suffer from his painful knee, and suffocate because of the laryngeal paralysis?
Or keep my opinion to myself, rather than going against a colleague’s advice?
After a week of mulling over this ethical dilemma, I gathered enough courage to call the owner. I was extremely hesitant. Was this even ethical?
I was convinced that I could help Puppy Magic, but what if something went wrong?
So we had a candid conversation. We discussed the facts. We weighed the pros and the cons. I very clearly explained the possible complications.
In the end, only Puppy Magic’s owner could make the final decision.
The additional difficulty was to decide which surgery to do first: the TPLO or the laryngeal paralysis surgery. Arguments could made either way…
After thinking about it, Puppy’s owner decided to take a chance, and put his dog’s future in my hands…
That’s a lot of pressure…
We eventually both agreed to start with the TPLO.
So in September of 2020, we did another TPLO, this time on the right knee.
Fortunately, thanks to the TLC and dedication of his owner, Puppy recovered smoothly.
Then in December of 2020, we did surgery to treat the laryngeal paralysis.
But wait, there’s more!
During his recovery, Puppy started to limp on the right FRONT leg. His family vet noticed some swelling of one of his toes. Long story short, there was a strong suspicion of cancer.
On the X-ray below, you can see 4 normal toe and 1 very swollen toe on the left (red arrow)…
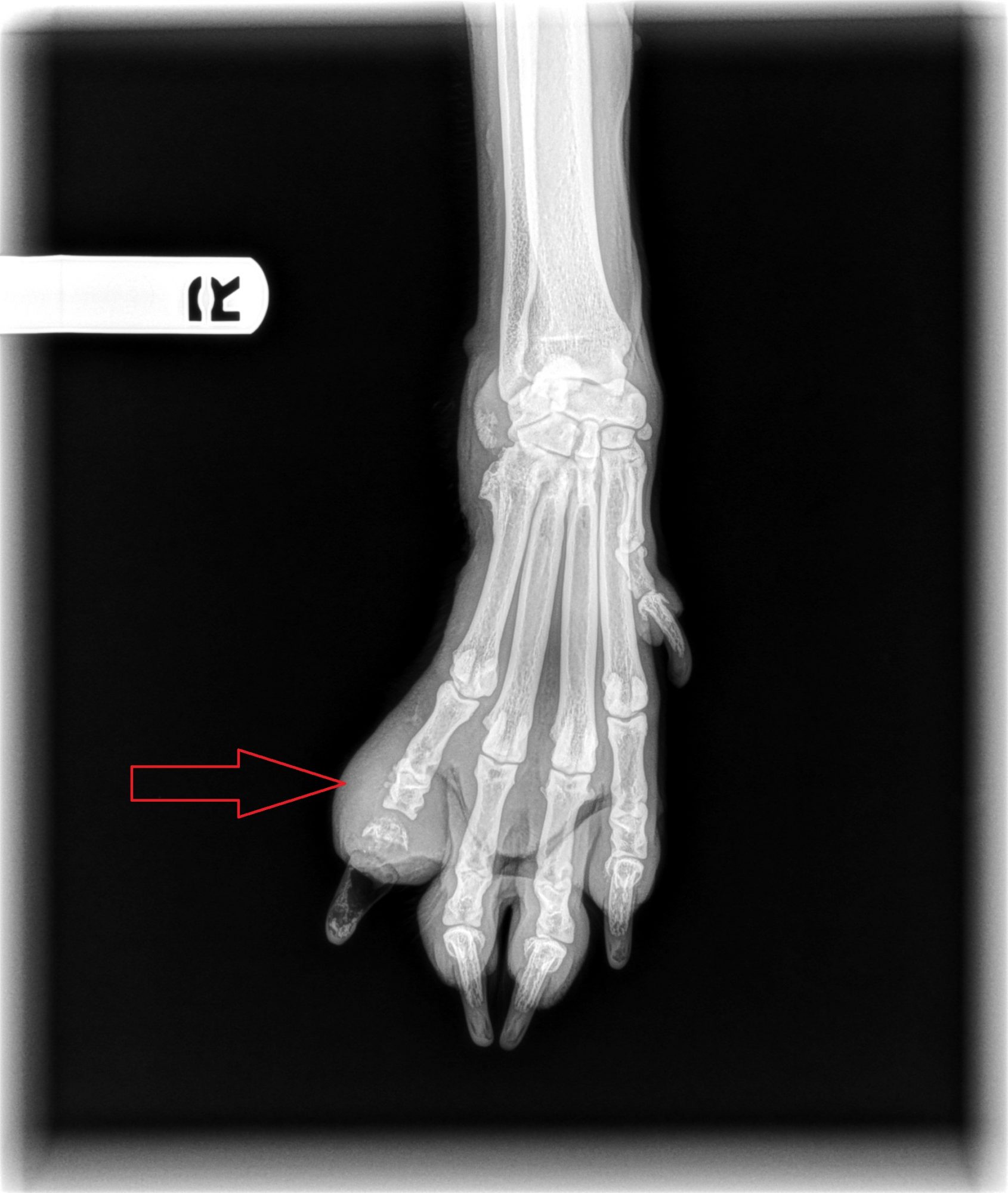
So here we went for yet another dilemma… Was it fair to do surgery? Was it ethical? When do we stop? What would you have done?
Again, Puppy Magic’s owner decided to give his pup a chance, and chose to go to surgery.
So, even though the clinic was in the middle of a giant snowstorm, we performed surgery to treat the laryngeal paralysis and amputated the toe.
Laryngeal paralysis causes difficult and noisy breathing.
The very next day after surgery, not quite used to the new situation, the owner wrote: “Breathing is good. I have to check Puppy’s stomach to see if he is breathing!”
That certainly was a good start!
One week after surgery: “He is walking much better – he has not walked this well in over 5 months.”
In addition, “Puppy is doing some good things he has not done in a while – like going into the kitchen to eat. His foot hurt too much before to do that.”
It’s the little things…
Sadly, 10 days after surgery, the diagnosis of cancer in the toe (squamous cell carcinoma) was confirmed. Fortunately, the cancer was removed 100%.

Two months after surgery, Puppy was finally done with healing. He was breathing well, wagging his tail, eating and drinking well, playful, eager to go on walks, and happy to be alive.
His owner concludes: “Puppy is doing great after his 4 surgeries. He has a great love of life and enjoys each moment.”
This story shows that when a family vet, a surgeon and a unusually dedicated pet owner work together, have open communication and trust each other, tricky situations, including cancer, can have a good outcome.
As of this writing, 6 months after his 4th surgery, Puppy Magic is still doing great.
Phil Zeltzman, DVM, DACVS, CVJ, Dear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
Squirrel gets a new lease on life after cleft palate surgery
Squirrel, a 2 year old bully mix, had an unusual problem.

She was struggling with eating and drinking on her own, as well as playing and chewing on toys.
Thick, white mucus would build up and make it hard for her to swallow or breathe through her nose.
Because of that, it was difficult for her to gain weight.
This is how she looked when she was first adopted.

Her foster explained: “She is choking & sneezing food and mucus out her nose every day, anytime she moves around, plays or chews on toys.”
“We almost lost her a few times the first year,” said her foster. “So she is a fighter for sure. She is a spunky little thing loving life!”
Her diagnosis? A cleft palate.
This means that there was a split in the roof of the mouth (similarly, a cleft lip is a split in the lip).
That split allowed food and water to go up in the nasal passages, causing difficulty breathing and constant infections.
That also meant that she could not get the proper nutrition her body needed to grow properly.
This is the reason why a puppy (or a kitten) with a cleft palate is typically the runt of the litter.
Now, a bit of anatomy. When you touch the roof of your mouth, it is firm because there is bone behind it. You are touching your “hard” palate.
PICTURES OF THE CLEFT BELOW ARE GRAPHIC AND ARE NOT FOR THE FAINT OF HEART.
The bone then disappears in the back of the mouth, so that part of the palate is called the “soft” palate.
Based on preop pictures, Squirrel clearly had a cleft of the hard palate.
The surprise came when we put her under anesthesia. A more thorough exam revealed a cleft in 100% of the roof of the mouth. So little Squirrel had a cleft of the hard palate and the soft palate.
In all of the pictures of the mouth below, Squirrel is on her back, and you see the inside of the roof of the mouth.
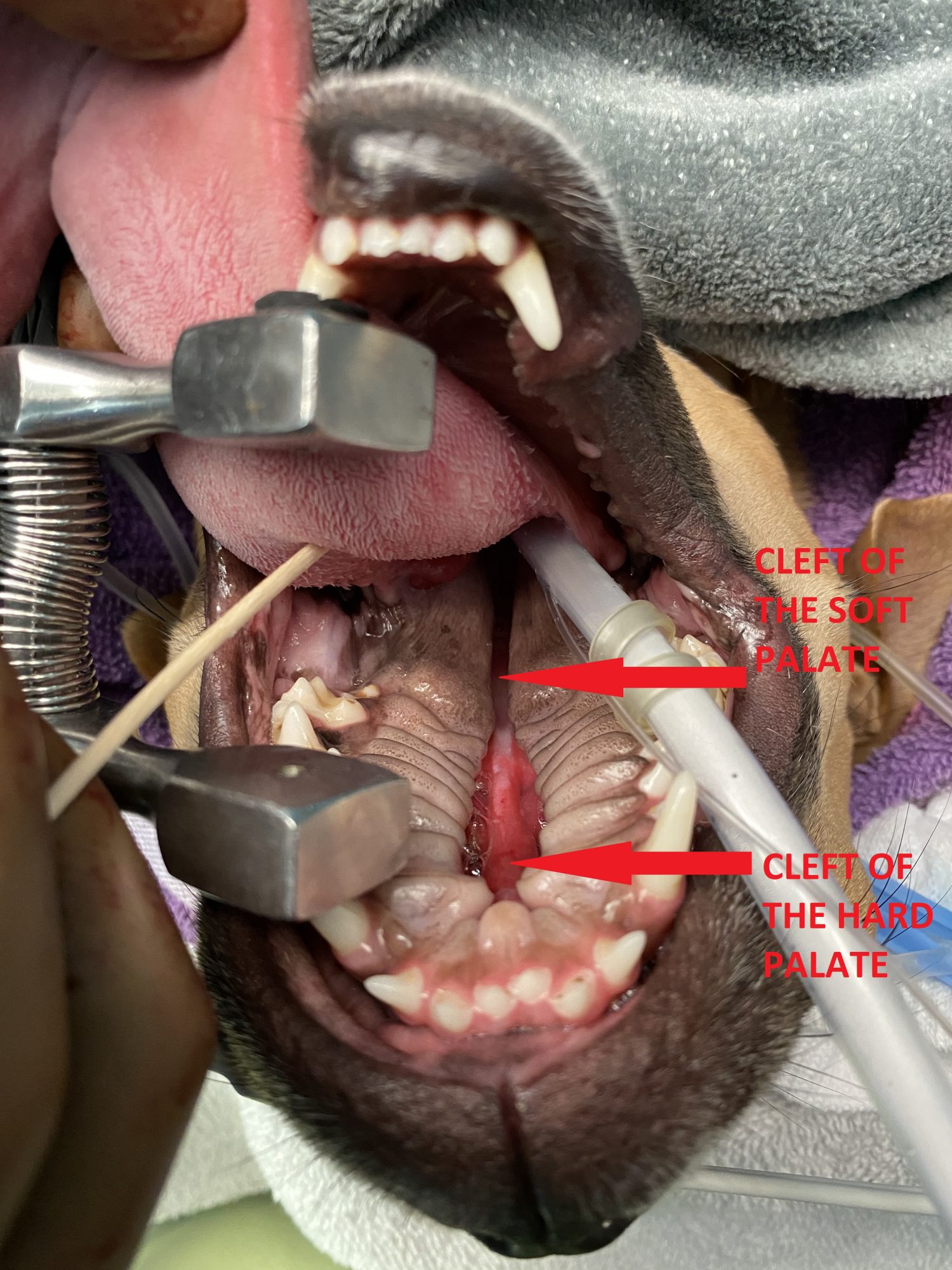
Surgery entailed stealing tissue from Peter to give to Paul.
WARNING: THE PICTURES BELOW ARE GRAPHIC, SO CONTINUE AT YOUR OWN RISK.
We created a “flap” by using healthy tissue from each side of the roof of the mouth to cover the defect or split in the middle.
In the end, we were able to cover the entire defect in the hard and the soft palate.
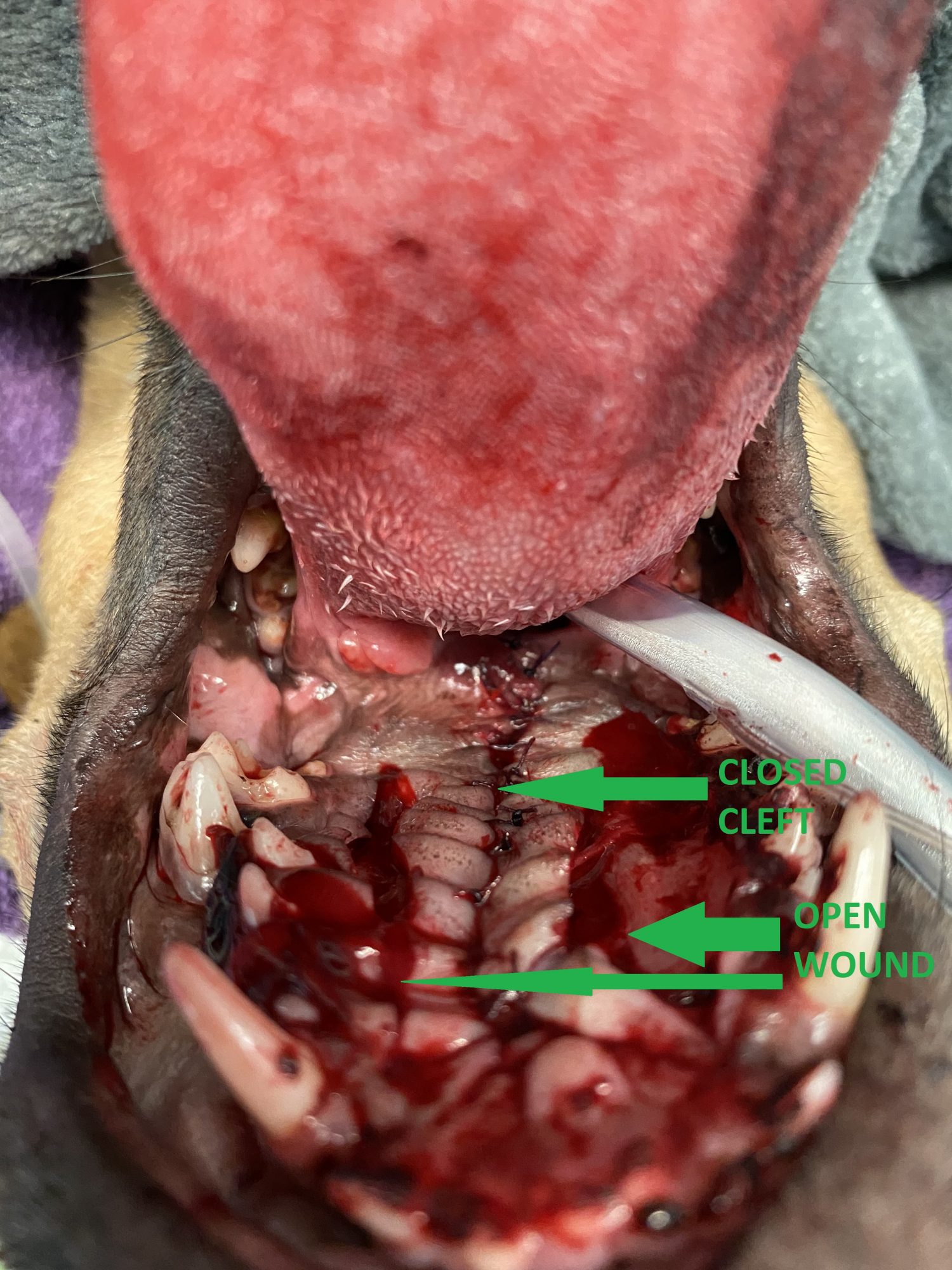
Squirrel went home safely the day of surgery.
She had to be kept quiet and away from chew toys and hard food for 3 weeks to protect the surgery site and the stitches.
Her foster took exceptional care of her… She did not spoil her at all as you can see in this picture…

Only two days after surgery, her foster commented: “She is eating watered-down canned food, and lots of it. She is also drinking better. Hardly any sneezes. She doesn’t seem painful. I am amazed at how well she is doing honestly!! She seems surprised she can breathe through her nose and not sneezing.”
Four days after surgery, she kept improving: “Squirrel is now eating soft can food. No water added. She ate half a can this morning.”
Three weeks after surgery, we examined her mouth under sedation to assess the surgery site.
Thankfully, 100% of the surgery area “took.” The left side of the mouth (the pink area) still needed a bit more time to heal as nicely as the right, but I was reassured that everything worked out after the first surgery.
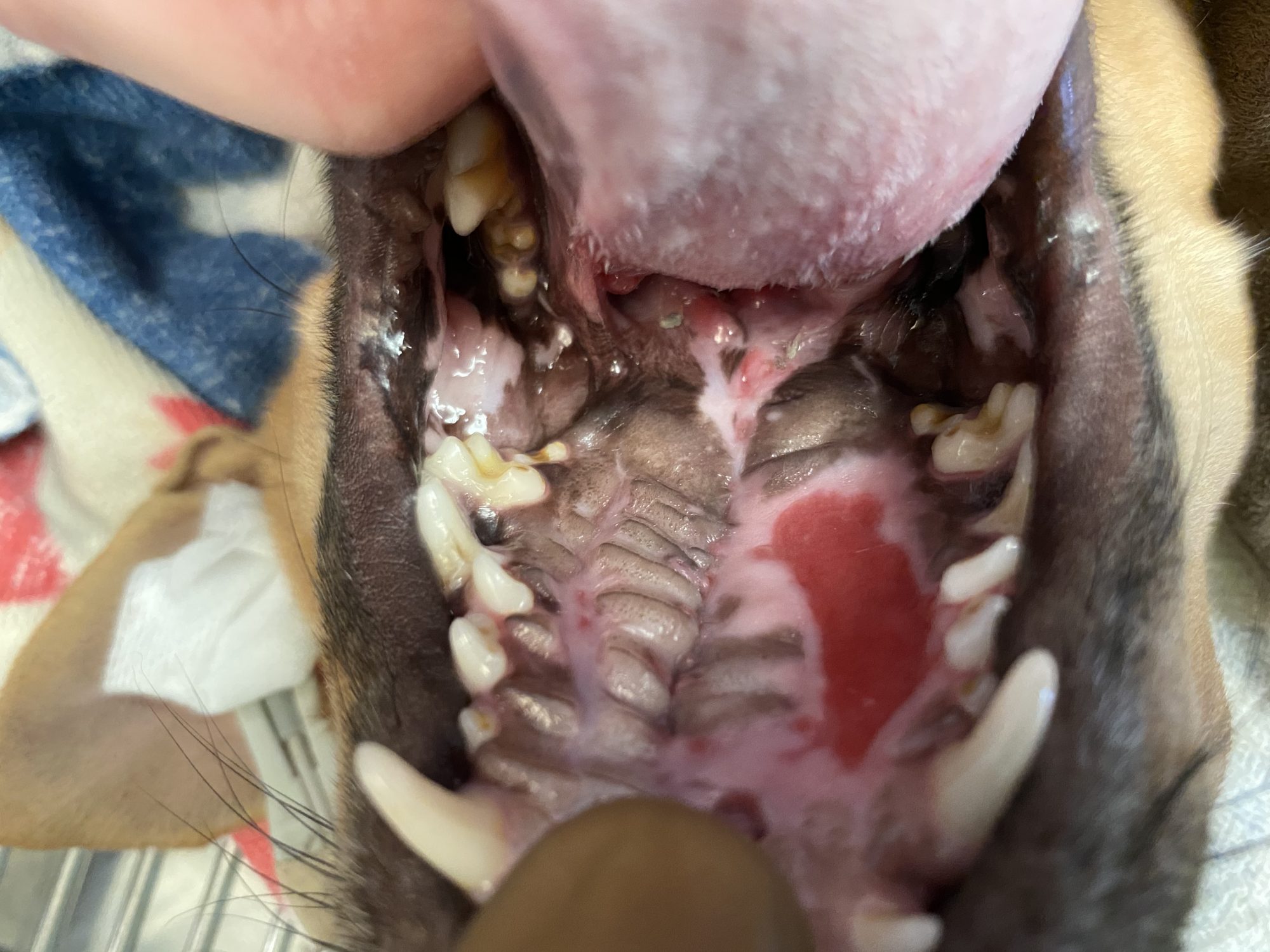
Squirrel’s foster concludes: “I cannot thank you enough for giving her this gift! She now has a new lease on life.”
Phil Zeltzman, DVM, DACVS, CVJ, FFcert.

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
You removed how much of Mimi’s jaw???
Mimi, a cute 9 year old miniature poodle, started to bleed from the left side of the mouth.

Initially, it was on and off, nothing scary. Then she started to drool after eating and drinking. Sometimes, the saliva was mixed with blood. When the bleeding became consistent, Mimi’s owner went to her family vet.
The conclusion was shocking: Mimi had a tumor in her left lower jaw bone (mandible). Her vet took X-rays (below), which showed that the front of the left lower jaw bone was eaten away by an aggressive tumor, which the back section of the jaw showed a growing tumor.
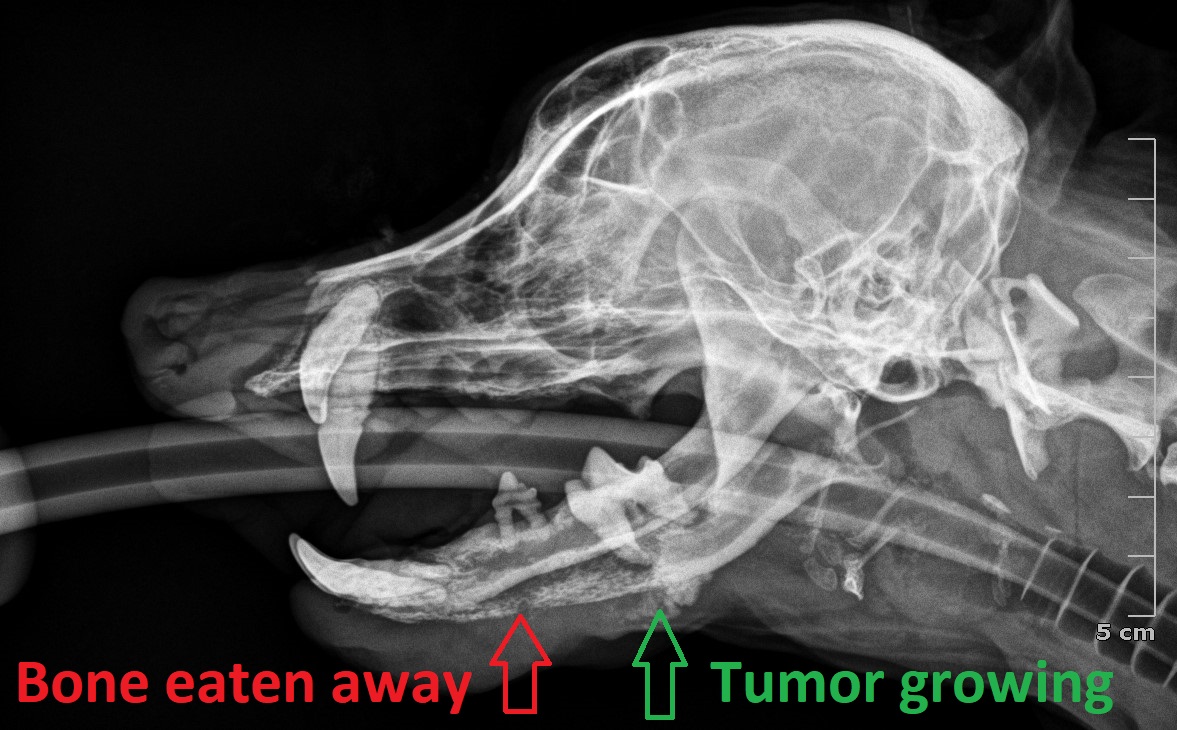
WHAT FOLLOWS IS GRAPHIC, SO YOU MAY WANT TO STOP READING IF YOU ARE A SENSITIVE SOUL.
Mimi was referred for surgery. It is necessarily invasive, because you can’t remove the mass only. The tumor was in the jaw, so part of the jaw, including the teeth, had to be removed. Removing part of the lower jaw or mandible is called a partial mandibulectomy. As drastic as it sounds, dogs look fairly good after this surgery. More importantly, they’re finally comfortable once the mass is removed.
Mimi’s owner drove all the way from from New York City to Harrisburg Regional Vet Surgical Specialty ( www.HRVSS.com ).
I had a long heart to heart with Mimi’s owner, trying to explain (along with pictures) how Mimi would look like after surgery. I kept saying: “It’s not for everybody.”
All Mimi’s owner wanted is to help her dog get comfortable.
On exam, it appeared that the mass had grown so much, that it had invaded the front of the jaw and extended to the right half of the mandible.
Now, that was a whole different story. Almost ALL of the mandible had to be removed. This is called a radical mandibulectomy. This is much more invasive and cosmetically dramatic.
I called Mimi’s owner and we had another heart-to-heart discussion. Again, I said: “It’s not for everybody.”
But Mimi’s owner was committed to doing anything to help her dog, knowing the possible risks and complications. So we proceeded with surgery.
Actually, before an invasive surgery, we needed to make sure the tumor had no spread to the lung (see X-ray below), which fortunately it had not.
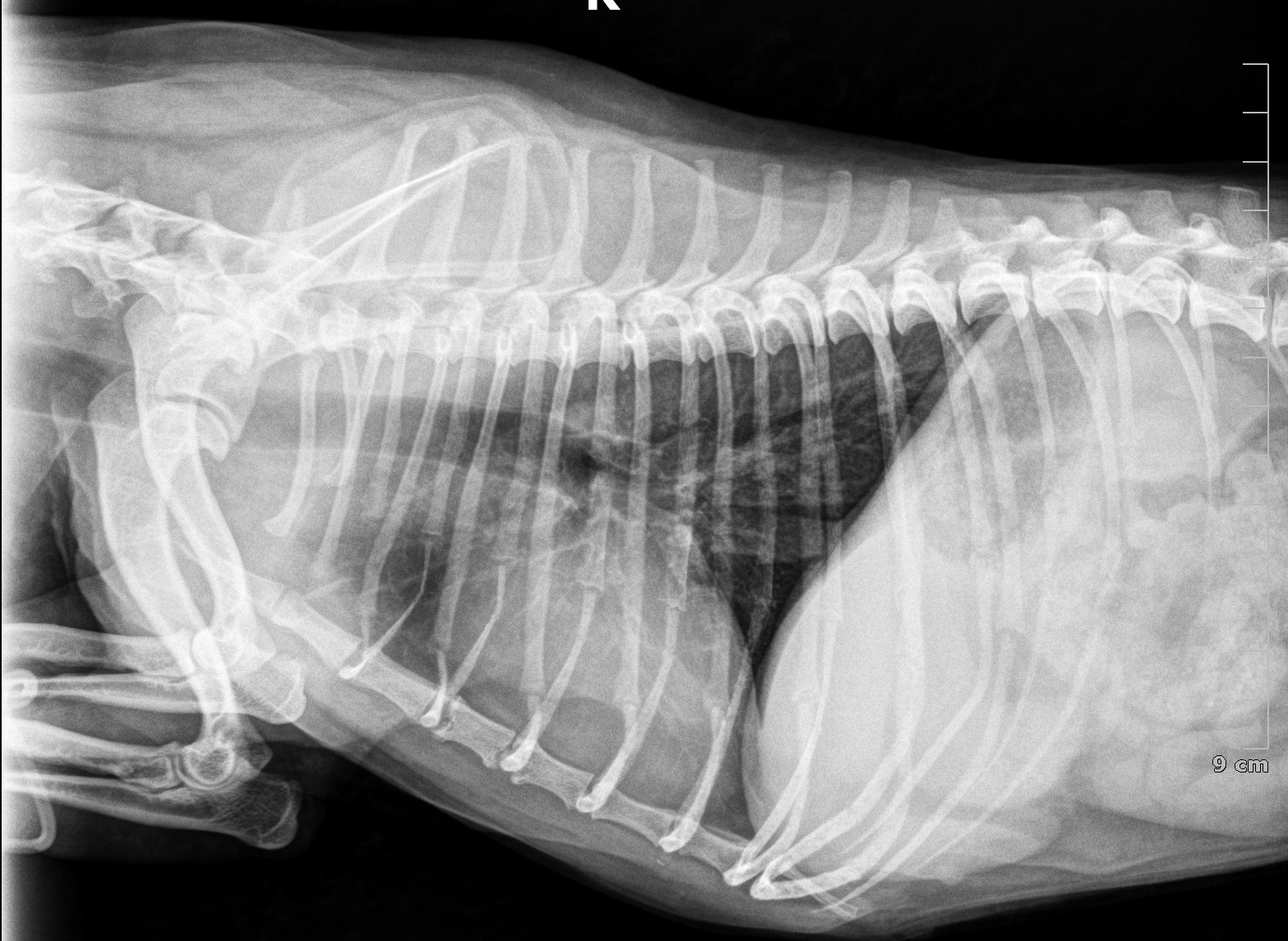
YOU HAVE BEEN WARNED, WHAT FOLLOWS IS NOT FOR THE FAINT OF HEART.
Surgery was uneventful. About 95% of the lower jaw was removed with no complications. Mimi recovered smoothly from anesthesia. She was kept overnight in the hospital, where she was monitored by a nurse, and received plenty of TLC.
Thanks to multiple types of pain medications given before, during and after surgery, she seemed very comfortable. So comfortable, that she ate 4 times that night!
Of course, she had to relearn how to eat, so things were a bit messy as you can see in the picture below.
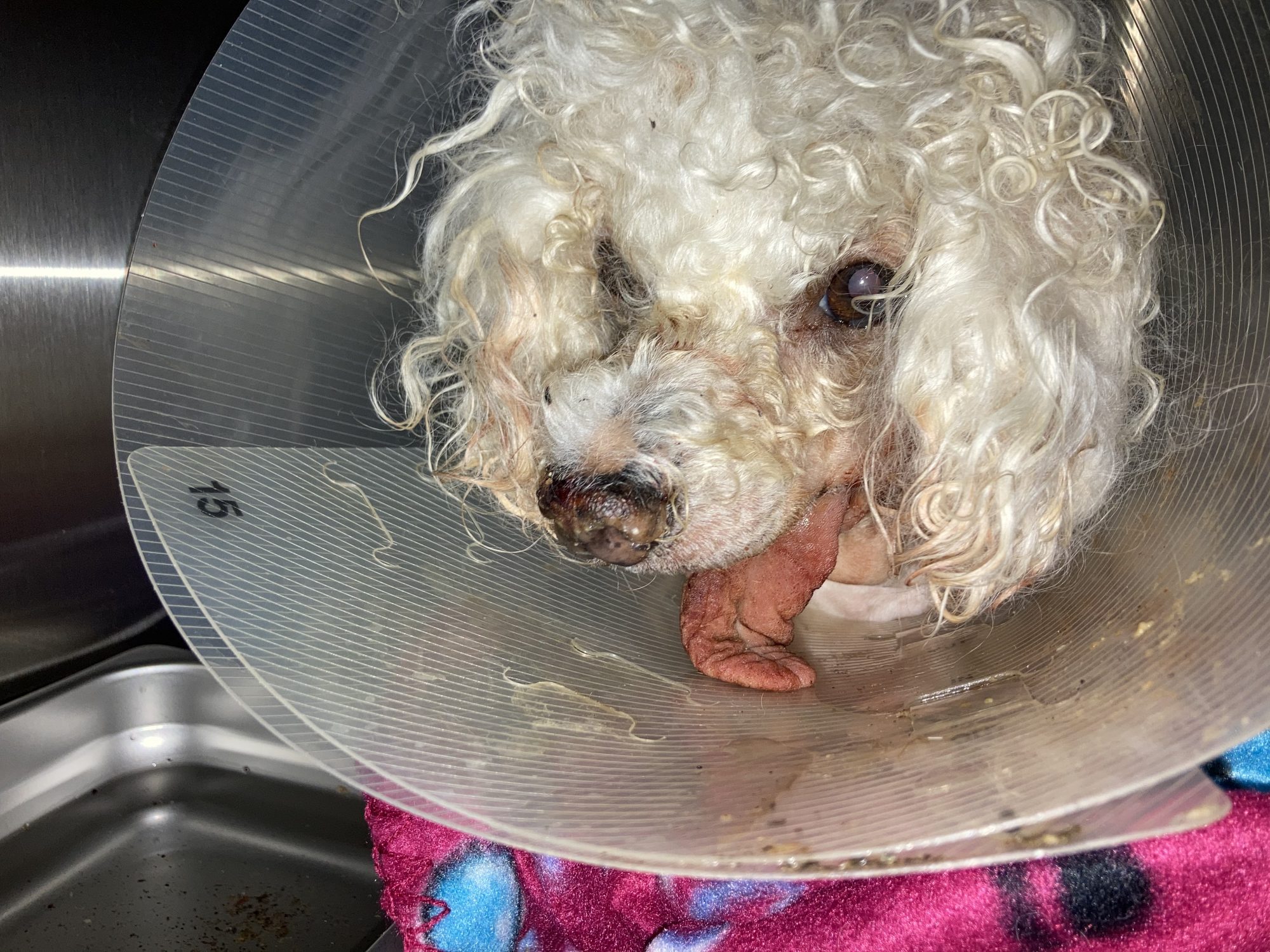
Mimi was discharged the very next morning.
The jaw was sent out to the lab for evaluation. The tumor was a squamous cell carcinoma, one of the most common types of cancer in the mouth (in cats and dogs).
Fortunately, the lab confirmed that we “got it all.”
Since surgery, Mimi has been home, where her owner took exceptionally good care of her.
Clearly, this surgery is not for everybody. It requires a very dedicated and loving pet owner who is willing to assist their pet with eating and drinking as needed, and who can get over the cosmetic appearance of their pet without judgment.
With modern surgery and generous pain medications, most pets do very well after invasive surgery, including removing a large part of the jaw.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
Laryngeal paralysis is not a death sentence
Laryngeal paralysis (aka “lar par”) is a common condition in dogs (and rarely cats). What follows are my thoughts about the condition, its treatment and its outcome. They are based on recent science, and many years of experience treating lar par.

What is Laryngeal Paralysis?
Laryngeal paralysis is a condition that severely affects a pet’s breathing.
In the veterinary world, we call it “Lar Par” in short. A few people call it LP.
The larynx (please note, it is larynx and not “lar-nynx” as many people call it…) is the medical name for the voice box. If you’ve ever had laryngitis, then your very own larynx was irritated. The larynx is also the entrance to the wind pipe (or trachea) and, beyond, to the lungs.
Besides making all kinds of noises, the job of the larynx is to close off after we inhale, open up when we inhale, and again shut off when we eat and drink so we don’t “swallow the wrong way.”
When laryngeal paralysis occurs, none of these things happen. Taking a deep breath becomes impossible. The poor dog literally suffocates.
Who can be affected?
The typical patient is an older large breed dog. The poster child is the Labrador.
Most dogs are over 10 years of age.
Males are affected 2-4 times more often than females.
There is a hereditary or congenital form of Lar Par, which can affect Bouviers des Flandres, Huskies and Dalmatians. In those rare cases, young dogs, 1 year or younger, are affected.
Lar Par has also been described in small to medium dogs, as well as cats.
To avoid posting a long list here, I’ve shared the list of breeds I’ve treated over the years at the bottom of this article*.
What happens?
Lar Par occurs because the nerves that control the muscles which act on the cartilages of the larynx are diseased.
Typically, the condition starts on one side (“unilateral” paralysis or hemiparesis). If your dog is an athlete or a working dog (racing, agility, police dog, serious hiking, Search And Rescue), you may notice breathing difficulties. But if your dog is a family pet or a couch potato, you probably won’t notice much.
Only when the condition affects both sides of the larynx (“bilateral” paralysis) will most pet owners realize that there is a problem.

What causes Lar Par?
Most of the time, we don’t know. This is called “idiopathic” Lar Par.
Occasionally, we find an underlying cause, such as hypothyroidism (a lazy thyroid). This is somewhat controversial, since hypothyroidism is common in older Labs and Goldens anyway. That said, treating hypothyroidism will never correct Lar Par. So we recommend treating hypothyroidism because of the other consequences, not because it helps or cures Lar Par.
Rarely, Lar Par is due to trauma, cancer, generalized diseases of nerves or muscles, or previous surgery (e.g. on the trachea or the thyroid gland).
What are the signs?
Lar Par is a very stressful condition for the patient — who obviously doesn’t understand what is going on. These dogs literally suffocate. It’s a terrible and terrifying condition.
Typically, the signs are progressive. The dog pants without exercising, has a noisy and labored breathing, and gets tired quickly during regular walks. Owners may notice that their dog’s voice changes and sounds hoarse.
Unfortunately, because Lar Par most often occurs in older dogs, the signs are often blamed on old age and arthritis… which delays treatment.
Therefore, Lar Par patients are often presented to a vet when they are in real trouble, i.e. when they can barely breathe. Most often, this happens as the weather becomes hot and humid, but I see these patients year-round, even in the Winter. Overweight or obesity worsens the condition.
At worst, the condition can become life-threatening.
How does my vet know my dog has Lar Par?
An experienced vet or surgeon will suspect Lar Par the second a patient walks into the exam room or on a 10 second video. But to confirm the suspicion, an exam of the larynx under sedation is necessary.
Before this can be done safely, we perform full blood work and chest X-rays. The purpose of blood work is to ensure the safety of sedation and anesthesia. The goal of chest X-rays is to know whether the patient has aspiration pneumonia (more on this below). The same X-rays can show if the patient as mega-esophagus, ie an enlargement of the esophagus – the tube between the mouth in the stomach. Finally, these X-rays confirm that there is no hidden cancer in the chest.
Under “light” sedation, the mouth is opened and the larynx is observed. With Lar Par, the folds of the larynx will not open and close as the patient breathes in and out. The folds remain closed – paralyzed.
Light sedation means that it should be heavy enough so the mouth can be opened, but mild enough for the patient to breathe spontaneously.
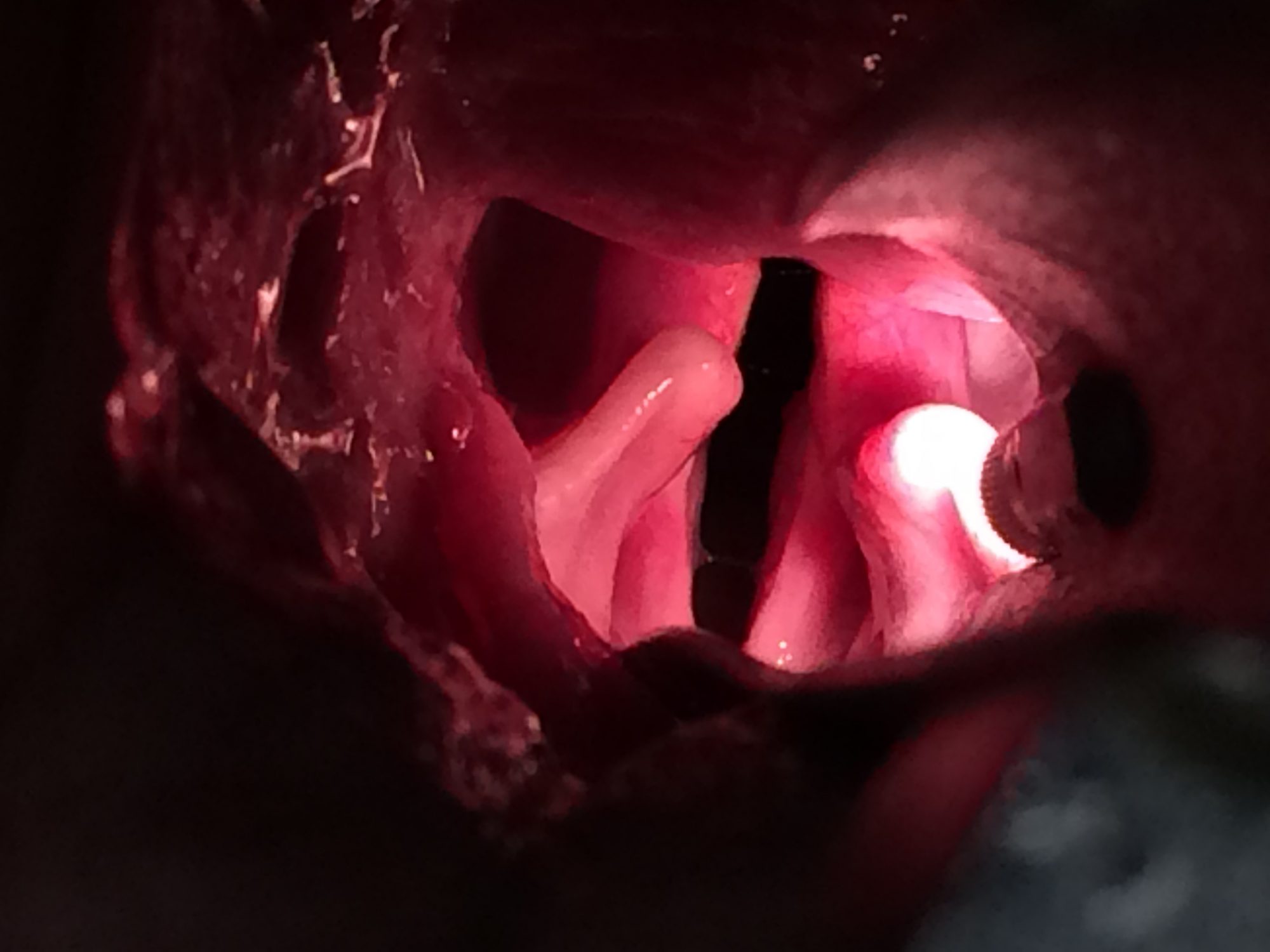
What is the emergency treatment?
When a patient presents on an emergency basis, two important goals are to calm the patient, and allow enough oxygen to get on board.
This requires sedation (acepromazine is often the drug of choice). Oxygen can be delivered by many different ways. In extreme cases, the patient needs to be anesthetized and a tube is placed down the throat to deliver oxygen.
My absolute least favorite way of stabilizing a Lar Par patient in crisis is an emergency tracheostomy, although it may be the only option in very rare cases.
If the patient’s temperature is seriously high from overheating, emergency measures are taken to lower it.
Once the patient is stabilized, surgery is the best treatment. Nothing else will work as successfully.
What happens in surgery?
The goal of surgery is to permanently open up the larynx to allow more air to get in.
There are two main types of surgery: intraoral (i.e. surgery is done via the mouth) and extraoral.
These days, the vast majority of surgeons will choose the extraoral approach, i.e. surgery is done through the left side of the neck. Most often, they will typically do a laryngeal “tie-back” procedure, a.k.a. arytenoid lateralization, on ONE side.
Typically, surgery involves placing 2 heavy nylon sutures (i.e. permanent) to open up the left side of the larynx. Only one side (again, typically the left) is opened up to minimize the risk of aspiration pneumonia.
Doing surgery on both sides dramatically increases the risk of aspiration pneumonia… and is simply not necessary.

What is the outcome?
In good hands, the outcome is typically good.
Theoretically, surgery provides instant relief: The patient can finally breathe. Then of course (s)he needs to recover and heal after surgery.
Clients often worry about doing this surgery in their (typically) older dog. The fact is, more lar par patients are over 10 years old.
My standard replies are:
1. Age is not a disease.
2. Lar Par is not a death sentence. It’s a bump along the road, which shouldn’t affect the patient’s life expectancy as long as they don’t get deadly aspiration pneumonia.
What are the complications?
. Coughing is expected after surgery, typically after eating and mostly after drinking. That’s a good thing, as it will hopefully prevent the dog from “swallowing the wrong way.”
. The voice may change, and barking disappears. These are not really complications. They are standard consequence of the tie back procedure you need to be aware of.
. Failure of the nylon sutures and/or a condition of the cartilage of the larynx (too soft or too brittle) are rare but severe complications, which is why we insist on confinement, peace, and quiet after surgery.
. The dreaded complication is Aspiration Pneumonia (also known as AP). This is a type of pneumonia due to aspiration, or inhalation, of food, water, saliva or vomit into the lungs. Thankfully it is an uncommon complication.
. GOLPP (geriatric onset laryngeal paralysis polyneuropathy) is not really a complication of lar par, but something to be aware of, especially in Labs. More information can be found here:

What if my pet gets aspiration pneumonia? Then what?
It’s crucial that aspiration pneumonia is caught early.
It is an aggressive disease that must be treated aggressively.
We look for 4 criteria: coughing, lethargy, poor appetite and a fever.
If you ever suspect AP, time is of the essence. A vet should see the patient ASAP, listen to the lungs and take chest X-rays to confirm the diagnosis. Treatment involves hospitalization, IV fluids, strong antibiotics, nebulization and a type of physical therapy called coupage.
What’s new with Laryngeal Paralysis?
We now give patients 2 anti-vomiting drugs (metoclopramide and Cerenia) and an antacid before surgery.
Then they stay on cisapride (a daily pill) for life, after surgery. The hope is to decrease the risk of vomiting by helping move food downward.
These days, we don’t make the opening in the larynx as big as we used to, just enough for the patient to breathe comfortably. This is clearly art more than science, and you can see how experience comes into play. What’s the downside? The patient will likely have a noisier breathing, as air goes through a smaller opening. But again, as long as the patient can breathe comfortably, we don’t mind. As I always tell my clients, “I don’t treat noise, I treat dogs.”

What do I need to do at home after surgery?
This will depend on your surgeon’s recommendations. In my practice, we recommend:
• Strict rest for 2 months to allow proper healing with scar tissue
• Soft food (“meat balls”) for 2 weeks
• Not too much water intake at once
• Pain killers for 7 days
• Cisapride for life (not all surgeons do that)
• Weight loss (these patients are often chubby), or weight control as needed
• A harness instead of a neck collar
The only restriction is swimming: your dog will have a permanently open larynx, with no possibility of closing it off, should (s)he swallows water. There is therefore a risk of aspiration at best, and drowning at worst.
What’s the bottom line?
Overall, Lar Par is a stressful condition for the dog and a stressful situation for the owner. Fortunately, in most cases, results of Laryngeal Paralysis surgery are good to excellent.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified
* Here is a list of breeds I’ve treated over the years:
Labradors and Lab mixes are # 1 by very very far.
Golden retriever
Pitbull
Greyhound
Shepherd (and mixes)
St. Bernard
Britany spaniel
Husky (young or old)
Sheltie
Beagle
Akita
Mastiff
Boxer
Bulldog (yes, really)
Pomeranian
Wheaten Terrier
Border collie
Springer spaniel
Chessie (Chesapeake Bay Retriever)
Bassett hound

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!
What is GOLPP (Geriatric Onset Laryngeal Paralysis Polyneuropathy)?
We used to believe that laryngeal paralysis was a standalone condition. Recent research shows that it’s a bit more complicated. Laryngeal paralysis is a disease of the nerves (poly-neuropathy) that can sometimes affect other body parts besides the larynx (voice box).

What is GOLPP?
To better describe this complicated disease, it was named Geriatric Onset Laryngeal Paralysis Polyneuropathy (GOLPP in short). GOLPP slowly gets worse over time. It affects dogs developing signs of upper airway obstruction or blockage.
It has been observed in older or geriatric dogs, particularly in Labrador retrievers and other large breed dogs. We now understand that there are 3 main parts to this disease.
* 1st condition: laryngeal paralysis
Affected dogs are most often brought into the hospital because of signs associated with laryngeal paralysis, because it’s the most obvious one and can be life-threatening. It causes dogs to have difficulty breathing, to the point that they can suffocate.
For more information on lar par, click here: Laryngeal paralysis is not a death sentence
* 2nd condition: mega-esophagus
Further questioning may reveal “spitting” up food, sometimes mistaken as vomiting (which is very active, ie lots of effort).
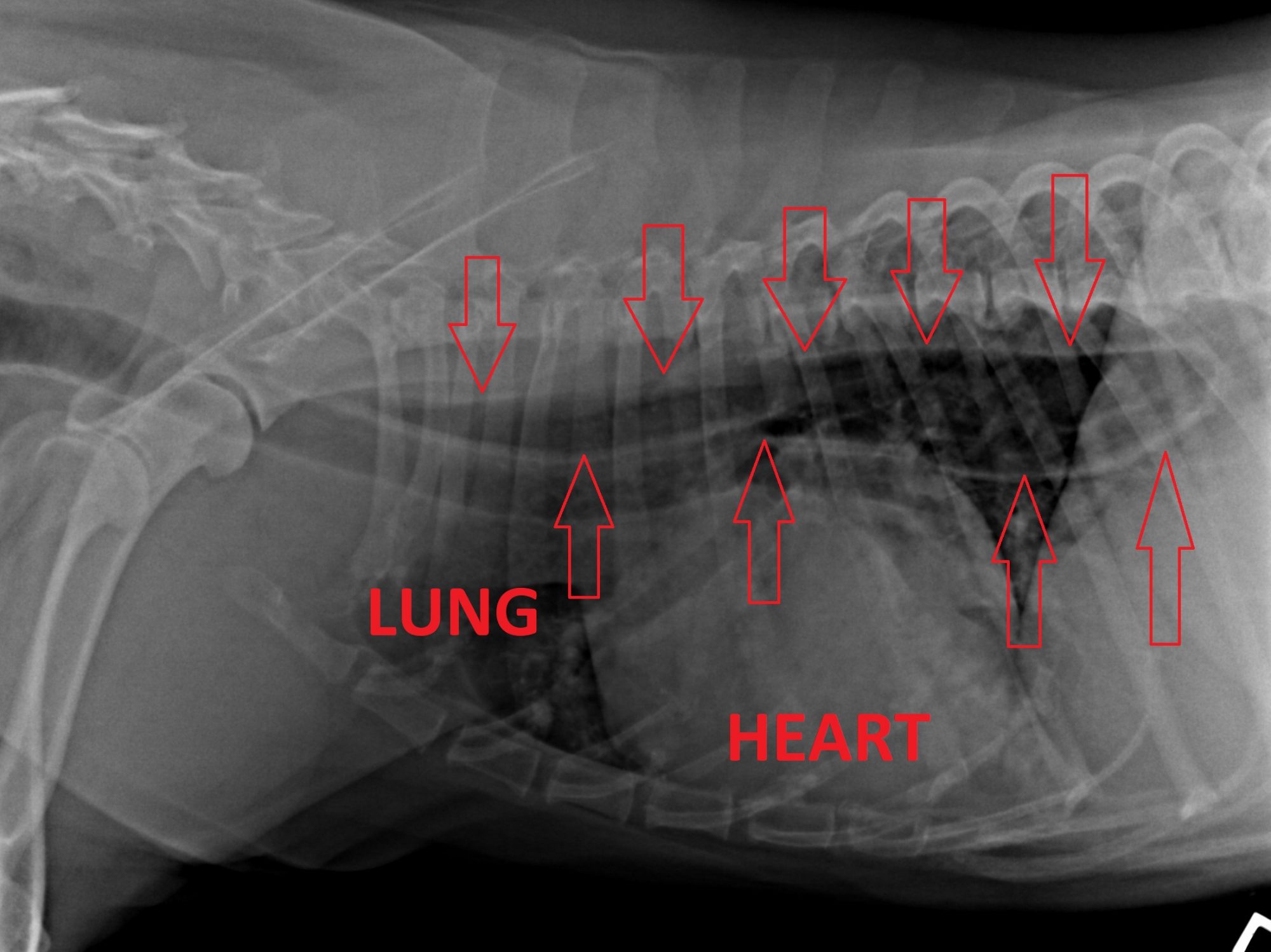
Because there is no effort involved, the condition is called regurgitation. It is due to a malfunction of the esophagus, which is the tube between the mouth and the stomach. It becomes extremely distended (mega-esophagus) and food simply piles up inside, instead of going down into the stomach. When the amount in the esophagus is too much, it’s expelled effortlessly via regurgitation.
This increases the risk of aspiration pneumonia since these dogs have trouble protecting their airways and lungs.
* 3rd condition: back leg weakness
In addition, some dogs develop weakness in their back legs. Sadly, it is often inaccurately blamed on arthritis or old age.
In reality, it really has to do with the same nerve condition. The legs are not well coordinated, and the muscles get weaker over time.
Which breeds are affected by GOLPP?
Most of the research has been done in Labradors. We know for a fact that Labs can get GOLPP. Some authors say that they all get it eventually. I think that it’s a bit more nuanced than that. I don’t think they all get it.
The condition has also been diagnosed in other purebreds and mixed breeds, but there isn’t as much research about them.
What is the treatment of GOLPP?
There is no cure for GOLPP, but there are ways to help each one of its components.
The gold standard to treat laryngeal paralysis is surgery (called a tie back). In good hands, i.e. typically those of an experienced board-certified surgeon, it provides good results as it allows the patient to breathe and function. Despite possible complications, surgery dramatically increases both lifespan and quality of life.
There is no treatment for megaesophagus per se. The dog needs to be fed soft to liquid food, then remain upright for 15 minutes after each meal.
Dogs with weak back legs benefit from slow leash walks and physical therapy to strengthen the muscles.

What should you do if your dog has GOLPP?
As a surgeon who deals with laryngeal paralysis & GOLPP frequently, this is what I tell my clients. Other surgeons may disagree, so please understand this is my personal & professional opinion, based on years of experience.
The best way to help a dog with laryngeal paralysis is surgery (a tie back). Suffocating is a horrifying way to live. Of the 3 different components of GOLPP, lar par is the one that affects quality of life the most, and the only one we can “fix.”
So my (again, personal) philosophy is: fix what can be fixed, and be ready to deal with what cannot be fixed (megaesophagus and weakness). It’s not for everybody. It requires serious love and dedication.
If the dog has megaesophagus at the time of the diagnosis, it still may not preclude performing surgery. It definitely increases the risk of aspiration pneumonia, but several of my most dedicated clients have helped their dogs successfully.
If the dog has a weak backend, at least this part is not life-threatening in the short term. With proper exercise and physical therapy, we can still help these dogs. And chances are, once a weak dog finally gets more oxygen, (s)he might get stronger after a tie back.
Ultimately, by putting together the right treatment plan and the right team, which includes a very loving and dedicated pet owner, affected dogs can maintain a good quality of life.
Phil Zeltzman, DVM, DACVS, CVJ, Fear Free Certified

Dr. Phil Zeltzman is a traveling veterinary surgeon in Pennsylvania & New Jersey. An award-winning author, he loves to share his adventures in practice along with information about vet medicine and surgery that can really help your pets. Dr. Zeltzman specializes in orthopedic, neurologic, cancer, and soft tissue surgeries for dogs, cats, and small exotics. By working with local family vets, he offers the best surgical care, safest anesthesia, and utmost pain management to all his patients. Sign up to get an email when he updates his blog, and follow him on Facebook, too!

